Malawi Priorities: HIV Treatment and Prevention
Technical Report
Key Messages
- Approximately 15% of new HIV and AIDS infections in individuals aged 15 years and over occur as a result of sex with female sex workers (FSWs), contributing to the spread of HIV and AIDS in Malawi. This points to the importance of targeting further programming toward the FSW community. Providing HIV services and support is key to stemming this stream of new infections in Malawi.
- A Comprehensive Ambipolar Package (CAP) which includes semi-annual testing, case management, pre-exposure prophylaxis (PrEP), and antiretroviral therapy (ART) adherence counseling to all FSWs would avert over 23,500 new infections to 2025 and 63,200 infections to 2030. It has a benefit-cost ratio (BCR) of 2.3, meaning that MWK 1 of investment generates MWK 2.3 of social benefits. It is the most cost-effective and impactful HIV and AIDS intervention analyzed in this report.
- Interventions that provide only ART adherence counseling to FSWs are similarly cost-effective with a BCR of 2.2. However, it averts substantially fewer infections than CAP: 14,500 new infections by 2025 and 35,300 by 2030.
- Interventions that provide PrEP alone were the least cost-effective of the three interventions analyzed. While the detailed outcomes of this stream are included in the analysis and technical report, they are not presented within the policy brief as this intervention stream involves high costs and lower outcomes.
- This report focused only on FSWs,1 and within this scope, the identified interventions yield only fair BCRs. We recommend careful consideration of alternative interventions to reduce the burden of HIV and AIDS before scaling up any of the interventions investigated in this report to ensure benefits are maximized per additional kwacha available.
Context
Malawi has made significant progress in the fight against HIV and AIDS. 90% of those living with HIV know their status and have been initiated on ART and 95% of pregnant women are screened for infection. Despite these notable successes, stemming new infections remains a concern in the country, with an estimated 32,300 annual new infections in 2019 alone according to the Global Burden of Disease. The continued importance of this issue was illustrated by its inclusion as part of the NPC Research Agenda in 2019.
Providing HIV and AIDS services to FSWs is one important lever to reducing the spread of the disease. This analysis indicates that interactions with FSWs contribute approximately 15% of new cases annually in those over the age of 15 - approximately 2,400 new infections among clients, in addition to those clients’ partners or partners, which loosely doubles the figure. Additionally, new entrants into the profession, typically younger women, are at extremely high risk of becoming HIV-positive within the first few years of work, adding to new infections as well as potential costs to the healthcare system throughout their lifetimes.
As of 2017, there were approximately 36,000 FSWs in Malawi with an estimated HIV prevalence of around 60%. FSWs face specific socio-cultural barriers, which add greater challenges in addressing HIV and AIDS for this High-Risk Group. For example, only 49% of FSWs report using condoms, citing among other reasons, clients’ unwillingness to use them. Limited economic opportunities for adolescent and young women, sub-optimal condom usage, and the migratory nature of FSW work set a challenging context for effective policy development in this arena, making effective use of available funding a critical piece in Malawi’s efforts to manage this issue.
Summary of Findings
Given the context on HIV/AIDS within Malawi, the research focused on three interventions, however for the purposes of this brief, the summary narrows that focus to the two most cost-effective options:
1. Comprehensive Ambipolar Package (CAP): This intervention is ambipolar (“working in two directions simultaneously”) in that it addresses the challenge from both the prevention and treatment sides. It includes the provision of PrEP and ART counseling for FSWs, as well as semi-annual testing, case management, and support services. Based on the results of the test, PrEP or ART would be provided through the health system.
2. ART counseling alone: As above but with only ART counseling provided. Without working alongside the provision of PrEP, the cost-savings here are reduced due to the continued inflow of new infections within the FSW population. Savings and benefits are accrued in the form of infections averted among those interacting with FSWs.
Avoided Infections as Benefits
If rolled out for 10 years, CAP avoids the largest number of infections at 63,200 to 2030, a third of which are FSWs themselves with the remainder their clients and sexual partners of clients. ART counseling alone leads to 35,300 avoided infections by 2030, all of which are clients of FSWs and their partners. The difference between the two approaches is that ART counseling alone addresses only one pathway to onward infection, whereas CAP addresses two: reducing the share of FSWs living with HIV that are able to infect others because their HIV viral load is unsuppressed and ensuring that HIV-negative entrants into the profession do not get the disease, reducing the overall pool of infected FSWs over time.
Figure 1: Cumulative Infections Avoided
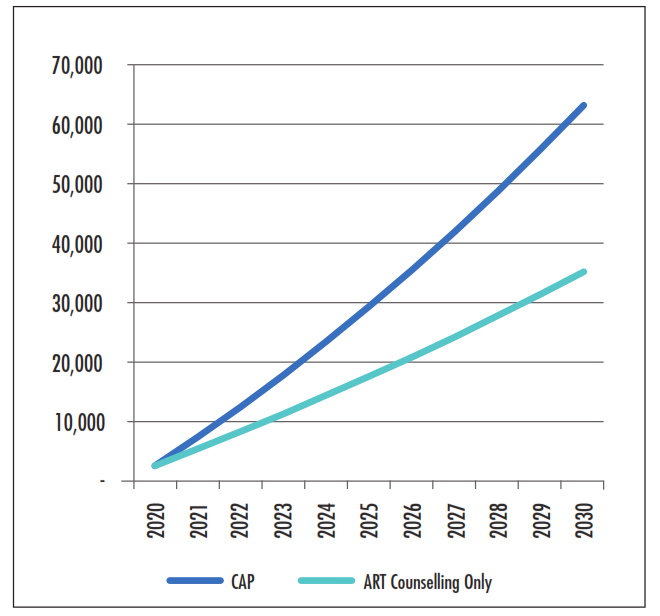
Avoiding infections leads to two main benefits
1. Avoided ART drug costs (estimated at MWK 112,000 per person, per year / USD 150), up to 52 years for FSWs and 38 years for other beneficiaries and,
2. Avoided mortality – concentrated among those who would not otherwise adhere to the ART regimen. To 2040,2 CAP would avoid 13,340 premature deaths while ART counseling would avoid 6,180 premature deaths. ART savings equal MWK 41 billion (USD 55 million) for the ART counseling alone intervention and MWK 79 billion (USD 107 million) for CAP. These ART savings start within one or two years. In both interventions, approximately two-thirds of the benefits up to 2040 accrue to the Malawian population as improved health and reduced health care costs. The remaining benefits are avoided ART costs, which accrue to the health system and ultimately the (future) funders of the HIV and AIDS program. In 2017, international and multilateral donors provided 95% of funding for HIV programs and would therefore reap these savings if this situation continued 10-20 years into the future.
Additional Government or Donor Investment Required
The additional government or donor investment required for ART counseling alone grows from approximately MWK 3.4 to 4.1 billion (USD 4.5 million to 5.4 million) annually between 2020 and 2030, amounting to a total of MWK 39 billion (USD 52 million) over 10 years — this represents an annual increase of approximately 2% over current funding of USD 222 million. The additional investment required for CAP grows from approximately MWK 5.7 to 8.7 billion (USD 7.6 million to 11.6 million) annually in 2030, amounting to a total MWK 77 billion (USD 103 million) over 10 years — equivalent to an annual increase of approximately 4% over current funding. The additional savings on ART will outweigh the increased program costs by approximately 2040.
Figure 2: Government or Donor Investment Required
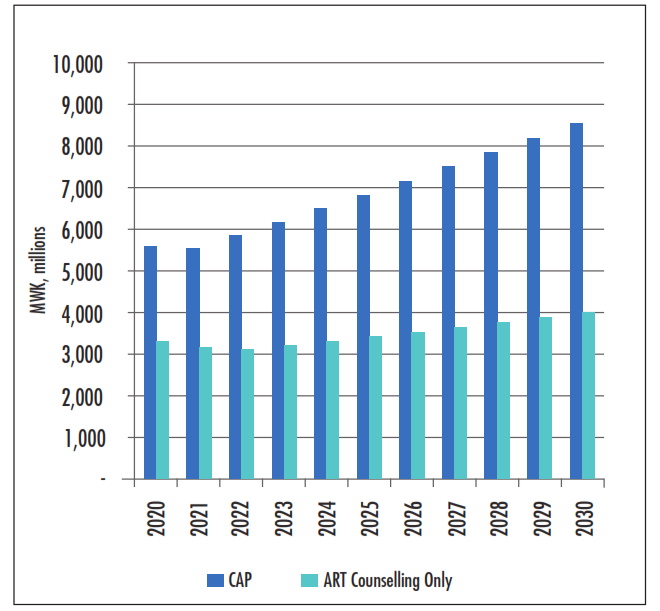
ART counseling generates almost immediate ART savings in clients and partners, which after the second year are larger than the additional costs of ART provided to FSWs. Within CAP, the additional costs primarily come from the provision of PrEP, which lowers or altogether nullifies new infections, and accordingly assists in lowering the number of FSWs requiring ART counseling over the long term. The costs per avoided infection are slightly larger for CAP than ART counseling alone. However, CAP has a slightly higher BCR because almost a third of the avoided infections are for FSWs who are younger on average and less likely to take ART, and the value of life-years saved is greater than the value of avoided ART costs. This means that avoiding infection in an FSW leads to more benefits than in non-FSWs. In contrast, ART counseling primarily generates benefits for non-FSWs.
Figure 3: Benefits of Comprehensive Ambipolar Program
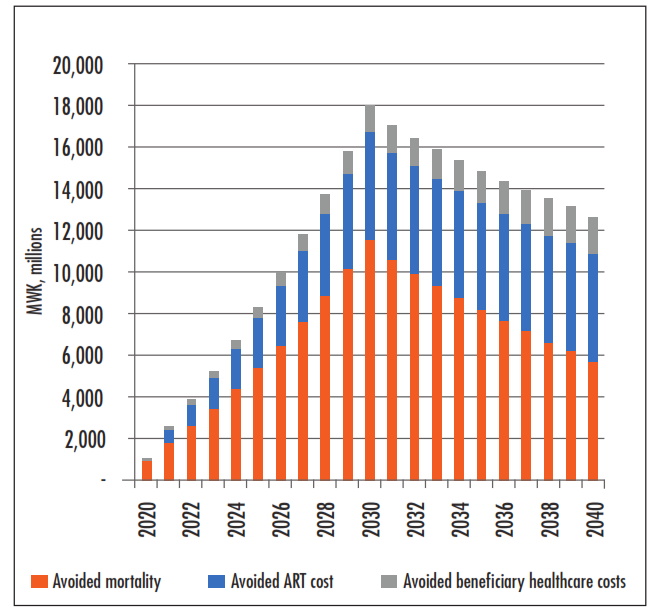
Summary Table
| Intervention | BCR | Target Group | Treatment Adherence | Averted Infections by 2030 | Cost per avoided infection | Additional govt / donor investment required to 2030 | Mortality avoided | ART savings | Payback Period |
|---|---|---|---|---|---|---|---|---|---|
| CAP | 2.3 Fair (100% economic benefit; 0% social benefit) | All FSW | 72% adherence to PrEP; 85% adherence to ART | 63,200 | MWK 1,200,000 (USD 1,627) | MWK 5.7 bn in 2020 rising to MWK 8.7 bn in 2030 | 13,341 deaths avoided to 2040 | MWK 0.6 bn in 2021 rising to MWK 5.2 bn in 2030 continuing into 2070 | Total ART savings exceed program costs in 2039 |
| ART counselling only | 2.2 Fair (100% economic benefit; 0% social benefit) | All FSW | 85% adherence to ART | 35,300 | MWK 1,300,000 (USD 1,756) | MWK 3.4 bn in 2020 rising to MWK 4.1 bn in 2030 | 6,177 deaths avoided to 2040 | MWK 0.8 bn in 2022 rising to MWK 2.3 bn by 2030 continuing into 2070 | Total ART savings exceed program costs in 2040 |
Note: BCRs are based on costs and benefits discounted at 8% (see accompanying technical report). BCR ratings are determined on the following scale Excellent, BCR > 15; Good, BCR 5-15; Fair, BCR 1-5; Poor, BCR < 1. This traffic light scale was developed by an Eminent Panel including several Nobel Laureate economists for a previous Copenhagen Consensus project that assessed the Sustainable Development Goals.
Download the full policy brief here.

